Rheumatic heart disease is more common in developing countries like India, where it is estimated to occur at a rate of 1.62 per 1,000 in the general population and constitutes 40% to 50% of all cardiac diseases.As a result, a large number of young women have undergone valve replacement before they conceive.
Pregnancy is associated with a hypercoagulable state as a result of various physiologic and biochemical changes that take place during this period. For women with mechanical valve prostheses, there is a general acceptance worldwide that subcutaneous heparin be used during the 1st trimester of pregnancy and oral anticoagulants for the remaining period until about 2 to 3 weeks before the expected delivery date, when the patient is switched back to heparin. Various studies have demonstrated that such a regimen is not entirely safe owing to lack of compliance, which may in fact pose a considerable risk to the mother’s life.Some studies have also suggested that the risk of fetopathy associated with warfarin use in the 1st trimester is overstated.
Types of Artificial Heart Valves
There are 2 types of prosthetic heart valves, bioprosthetic and mechanical. Although successful pregnancies are possible for women with prosthetic heart valves, there are potential complications—some of which can be fatal—for both types of valves.
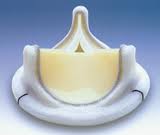
Bioprosthetic Heart Valve
Women who have well-functioning bioprosthetic heart valves and who do not have other cardiac risk factors often have uncomplicated pregnancies. One advantage of bioprosthetic valves is that they are much less thrombogenic than mechanical valves; however, there is still a risk of thromboembolic complications. The main issues with bioprosthetic valves is their finite lifespan and their risk of structural valve deterioration (SVD).Serious SVD can require reoperation to replace the failing bioprosthetic valve.Overall, about 50% of women of childbearing age will require valve replacement owing to SVD 10 years after the original operation; therefore, women of childbearing age who have bioprosthetic valves will likely require reoperation
Mechanical Heart Valve
Mechanical valves have excellent durability and SVD does not occur.In addition, newer-generation mechanical valves have superior hemodynamic profiles compared with stented bioprosthetic valves. All mechanical prosthetic valves, however, are thrombogenic and require lifelong anticoagulation to prevent thromboembolic complications.In addition, pregnancy is a hypercoagulable state. Examples of the types of thromboembolic complications that have occurred during pregnancies associated with mechanical prosthetic valves include stroke, valve thrombosis, and myocardial infarction.Choosing which type of anticoagulation to use during pregnancy is problematic, as there is no perfect form available. Therefore, the major concerns associated with pregnant women with mechanical heart valves are thromboembolic complications (including fatal events), maternal bleeding, and increased fetal events.
Anticoagulation therapy
The types of anticoagulation that can be used during pregnancy include warfarin, unfractionated heparin, and low-molecular-weight heparin (LMWH)
Warfarin
Warfarin is the drug of choice in nonpregnant patients with mechanical heart valves and is highly effective in preventing thromboembolic complications. In pregnant women, it can cause a specific embryopathy, consisting of nasal hypoplasia and epiphyseal stippling, albeit only when administered between 6 and 12 weeks of gestation.In a recent critical review of the available published literature, the authors estimated that the true incidence of warfarin embryopathy with exposure between 6 and 12 weeks of gestation was low( 5%); this contrasted with estimates of 30% or higher.Further, in recent follow-up studies of children born with warfarin embryopathy, major morbidity was uncommon, and many of these infants developed normally.
Other problems, such as fetal central nervous system abnormalities, have been reported in association with warfarin use at any stage of pregnancy.However, these events are rare and it is unclear whether the incidenceof any of these complications is higher than in pregnancies not associated with warfarin use. Finally, since warfarin crosses the placenta, maternal use can cause fetal hemorrhage, particularly during and immediately after delivery.However, this is likely to be rare and can be avoided by using a heparin (instead of warfarin) for the last part (2-4 weeks) of pregnancy.
Unfractionated Heparin
Since it does not cross the placenta, UFH is not teratogenic. However, multiple reports of thrombosed valves with the use of UFH,causing maternal morbidity and mortality, have raised seriousconcerns about its effectiveness.One plausible explanation for the failure of UFH is inadequate dosage. It is known that low-dose heparin(5000 IU every 8-12 hours subcutaneously) is inadequate for prevention of thrombosis of mechanical prosthetic heart valves during pregnancy; it is unclear whether 12-hourly subcutaneous UFH adjusted to prolong a midinterval activated partial thromboplastin time (aPTT) result to 1.5 to 2.5 times control is adequate. After initial heparin therapy, this regimen has been shown to be as effective as warfarin (with a target international normalized ratio [INR] of 2.0-3.0) for the prevention of recurrence in nonpregnant patients with acute venous thromboembolism.However, based on several considerations, this regimen of UFH might be less effective in pregnant women with mechanical heart valves.
First, 1.5 times control, the usual lower limit of the therapeutic range, corresponds to subtherapeutic heparin levels (anti-factor Xa levels 0.3 U/mL)using most currently available a PTT reagents.
Second, except for patients who have bileaflet mechanical aortic valvesand do not have atrial fibrillation, the recommended target INR range for patients with mechanical heart valves (2.5-3.5) is higher than the corresponding target INR range for the treatment of acute venous thromboembolism (2.0-3.0), suggesting that more intense antithrombotic therapyis appropriate.Further, although warfarin, with a target INR of 2.0 to 3.0, is highly effective in the long-term treatment of acute venous thromboembolism, even with the use of a more intense warfarin regimen (INR of 2.5-3.5), theaddition of aspirin to the warfarin regimen improves efficacy for patients with mechanical heart valves (albeit at the cost of an increase in the rate of minor bleeding).Given this information, we recommend that if subcutaneous UFH is used to prevent thrombosis in pregnant women with mechanical heart valves, the starting dose should be high(17500-20000 U every 12 hours) and adjusted aggressively to achieve a mid-interval aPTT of at least 2.0 timescontrol or a result that corresponds to an anti-factor Xa heparin level of at least 0.3 to 0.5 U/mL. Finally, adjunctive aspirin therapy should be considered in high-risk women,such as those with previous systemic embolism and those with atrial fibrillation.The rate of major bleeding in pregnant patients treated with UFH has been reported to be approximately 2%, which is consistent with the reported rates of bleeding associated with heparin therapy in nonpregnant patients and with warfarin therapy when used for the treatment of deep vein thrombosis.Unfortunately,adjusted-dose subcutaneous UFH can cause a persistent anticoagulant effect at the time of delivery, which can complicate its use prior to labor.
Approximately 3% of nonpregnant patients receiving UFH develop immune, IgGme d i a t e d t h r omb o c y t o p e n i a , wh i c h i s f r e q u e n t l y complicated by extension of preexisting venous throm-boembolism or new arterial thrombosis.In pregnant women, the true incidence of IgG-mediated thrombocytopenia is unknown. Long-term heparin therapy has been reported to cause osteoporosis in both laboratory animals and humans.Further, symptomatic vertebral fractures have been reported to occur in about 2% to 3% of patients receiving UFH for periods of 1 month or more and significant reductions in bone density have been reported in up to 30% of patients receiving long-term UFH.
Low-Molecular-Weight Heparin
The true incidence of valve thrombosis in enoxaparin- (orother LMWH-) treated pregnant women with mechanical heart valves and the optimal LMWH treatment regimen fortheir patients are unknown. Based on published data, there have been a small number of patients treated with LMWH,most successfully.The small numbers of patients withvalve thrombosis in the randomized trial of enoxaparin (2 of7, 29%) have very wide confidence intervals (4%-71%) and,when combined with the limitations of the postmarketingdata, preclude an accurate estimate of the true rate of fataland nonfatal valve thrombosis despite the information contained in the recent “Precaution” and “Dear Health CareProfessional” letter.The potential for teratogenicity of LMWHs lacks biologic plausibility because it has been demonstrated that these agents do not cross the placenta. In support of this,a recent comprehensive overview concluded that therewas no teratogenicity associated with LMWHs.
TREATMENT RECOMMENDATIONS
Women with mechanical heart valves should be carefully counseled about the risks associated with available anticoagulant options prior to, or shortly after, becoming pregnant. The practice of substituting warfarin with UFH or an LMWH between 6 and 12 weeks of gestation probably eliminates the risk of warfarin embryopathy (or other teratogenic effects) but might subject women to an increased risk of thromboembolism if inadequate dosesare used.One of the following approaches is recommended:
1. “Aggressive” adjusted-dose UFH throughout pregnancy; ie, administered subcutaneously every 12 hours in doses adjusted to maintain the mid-interval aPTT at a minimum of twice control or an anti-factor Xa heparin level of at least 0.3 U/mL.
2. Adjusted-dose LMWH throughout pregnancy; ie,administered subcutaneously every 12 hours in doses adjusted to maintain a 4- to 6-hour post injection antifactor Xa heparin level at a minimum of 0.5 U/mL.
3. UFH or LMWH (as above) until the 13th weekof pregnancy, then warfarin with a target INR of 2.5 to 3.5 until the middle of the third trimester, followed byreinitiation of UFH or LMWH until delivery.
With any of the 3 above regimens, adjunctive aspirin therapy should be considered. Long-term anticoagulants should be resumed post partum with all regimens
Prognosis
There have been several studies looking at the outcome of pregnancies in women with prosthetic heart valves.Women with mechanical valves have a higher complication rate, including the increase of both maternal and fetal events,compared with women with bioprostheses. Women with bioprostheses who are not using anticoagulation have been found to have excellent fetal outcomes.When compared with women with bioprosthetic valves, women with mechanical heart valves have a higher incidence of pregnancy loss, premature births, maternal deaths, thromboembolic complications, and bleeding.Women with bioprosthetic valves, however, have been found to have a higher incidence of structural valve failure, often occurring when both mothers and babies are still young.
Precaution
Women who have prosthetic heart valves and are of childbearing age should be counseled (ideally before conception) about the potential issues that might arise during pregnancy. Having a prosthetic heart valve puts both the mother and fetus at risk; therefore, management of these women is required throughout pregnancy in a specialized program for high-risk patients by a Cardiology team of doctors.









1 comment:
Severe valve damage means that the valve will need to be replaced. Heart valve replacement surgery is most often used to treat aortic valves and severely damaged mitral valves. Heart valve replacement surgery in Indiais a popular solution to get rid damaged valves in clinical, yet safe, friendly, and relaxing manner with assurance to get the best possible result.
Herniated disc surgery in Indiahas become a specialty. It combines the latest innovations in medical electronics with unmatched expertise in leading neurosurgeons and spine surgeons. Indian spine centers have the distinction of providing comprehensive spine care spanning from basic facilities in preventive back-care to the most sophisticated curative technology.
Valve replacement surgery india
HCG Hospital Bangalore
Herniated disc surgery in india
Robotic heart surgery India
robotic heart bypass surgery India
Post a Comment